Articles
- Page Path
- HOME > J Educ Eval Health Prof > Volume 11; 2014 > Article
-
Research Article
Handover practice amongst core surgical trainees at the Oxford School of Surgery -
Hazim Sadideen1*
 , Karim Hamaoui2
, Karim Hamaoui2 , Munir Saadeddin3
, Munir Saadeddin3 , Lucy Cogswell4
, Lucy Cogswell4 , Tim Goodacre4
, Tim Goodacre4 , Tony Jefferis5
, Tony Jefferis5
-
DOI: https://doi.org/10.3352/jeehp.2014.11.3
Published online: February 28, 2014
1Department of Plastic and Reconstructive Surgery, Queen Elizabeth Hospital, University Hospitals Birmingham NHS Foundation Trust, Birmingham, United Kingdom
2Department of Renal Medicine and Transplantation, Hammersmith Hospital, London, United Kingdom
3Department of Orthopaedic Surgery, King Saud University, Riyadh, Saudi Arabia
4Department of Plastic and Reconstructive Surgery, John Radcliffe Hospital, Oxford University Hospitals NHS Trust, Headley Way, Headington, Oxford,United Kingdom
5Oxford Deanery Postgraduate School of Surgery, Oxford United Kingdom
- *Corresponding email: hazim.sadideen@doctors.org.uk
©2014, National Health Personnel Licensing Examination Board of the Republic of Korea
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 56,017 Views
- 147 Download
Abstract
-
Purpose:
- To date no studies have specifically evaluated the use of handovers amongst core surgical trainees (CSTs) in the United Kingdom. We examined handover practice at the Oxford School of Surgery to assess and improve CSTs’ perception of handover use as well as its quality, and ultimately patient care.
-
Methods:
- Based on guidelines published by the British Medical Association and Royal College of Surgeons, a 5-point Likert style questionnaire that collected data on handover practice, its educational value, and the CSTs’satisfaction with handover was given to 50 CSTs in 2010.
-
Results:
- Forty CSTs (80.0%) responded to the questionnaire. The most striking findings revolved around the perceived educational value, formal training, and auditing practice of handovers throughout various units, which were all remarkably lower than expected. As a result, handover practice amongst CSTs was targeted and revised at the University Hospital’s Department of Plastic Surgery, with the implementation of targeted changes to improve handover practice.
-
Conclusion:
- The execution of daily handovers was an underused educational tool amongst surveyed CSTs and may be an important modality to target, particularly in the competency-based, time-limited training CSTs receive. We recommend modifications to current practice based on our results and the literature and encourage the assessment of handover practice at other institutions.
- The National Patient Safety Agency in the United Kingdom (UK) defines handover as “the transfer of professional responsibility and accountability for some or all aspects of care for a patient, or groups of patients, to another person or professional group on a temporary or permanent basis”[1]. Handover is a complex process that occurs in multiple settings, at various hours, and between and within multiple health and allied health professional groups; therefore, handover practice is a recognised issue in maintaining patient safety.
- Handover in surgical care is topical. After initiation of the European Working Time Directive (EWTD) and New Deal in the UK, junior doctors do not normally more than 48 hours per week[2]. One of the goals in reducing working hours amongst trainees is to reduce the rates of medical and surgical errors due to potential fatigue from excessive on-call commitments[3]. To facilitate this reduction in working hours, a transition has been made from an on-call system to a shift-based rota.
- Appropriate handover of patient responsibility and care between staff has continued to be an integral part of good medical care. However, with the introduction of shift-based systems, several different groups of healthcare professionals might now be responsible for patient care over a 24-hour period, thus resulting in several 'handovers' of care. Thus, the role of handovers has diversified to reflect the need for compliance with working time directives as well as focus on its primary role of maintaining continuous patient care by transferring responsibilities between staff as shifts change. The Royal College of Surgeons of England identifies formal and appropriate handover as a core component for the delivery of safe patient care[4]. To preserve patient safety during handover, the British Medical Association (BMA)[1] and the Royal College of Surgeons of England[5] published national guidance on the conduct of safe clinical handovers. Briefly, these guidelines state that safe clinical handovers should be led by a senior clinician encouraging interaction between team members as a focused, structured multidisciplinary session of adequate duration. Moreover, handovers should take place in a consistent location that prevents interruptions and should be timetabled into shift-based rotas. These guidelines also suggest that local handover practice be regularly audited as an integral part of clinical governance strategies.
- Overall, handover is an important professional process where clinical teams meet, communicate, interact, provide mutual support, and enable learning[6]. In the era of the EWTD, effective handover can play a substantial role in maximizing educational perspective, whilst maintaining adequate service provision. Thus, assessment of handover practice use amongst current core surgical trainees (CSTs) in the UK would be beneficial to understanding and improving its role. The first aim of our survey was to determine the status of handover practice amongst CSTs (from core training levels 1 to 3) at the Oxford School of Surgery, and the second aim was to investigate their perception of the efficacy and regional educational value of the handover process and its influence on patient safety.
INTRODUCTION
- This study was approved by the local audit department. A questionnaire-based survey was designed in line with the guidelines of the Royal College of Surgeons of England and BMA. The survey collected data on handover practice and policy as well as the perceptions of the CSTs regarding handover efficacy, patient safety, and its educational value in surgical training. The surveyed population included all CSTs at the Oxford School of Surgery (n=50) who worked in any hospital or surgical specialty within the region between January and April 2010. CSTs were asked to complete the questionnaire in relation to their surgical specialty during the survey period. The questionnaire (Appendix) was emailed a maximum of two times to non-responders. Information regarding timing, location, duration, data transfer methods, formal policy, attendance/participation, quality, and the educational value of local handover practice was collected. Each item was assessed using a 5-point Likert scale (5, strongly agree and 1, strongly disagree). Questionnaire data was divided into the following categories: (1) handover practice and patient safety, (2) policy and training, and (3) educational value. Participants did not receive an incentive, and all information was collected anonymously. Data was transferred, verified, and stored in a security-protected database. Following analysis of this data in March 2011, major changes were implemented to improve handover practice in the Department of Plastic Surgery at the John Radcliffe Hospital (Oxford, UK).
METHODS
- Forty questionnaires (80.0%) were fully completed by the CSTs. These trainees represented six surgical specialties (urology, general surgery, cardiothoracic surgery, plastic surgery, trauma, orthopaedic surgery, and neurosurgery) across seven hospitals.
- Status of handover practice
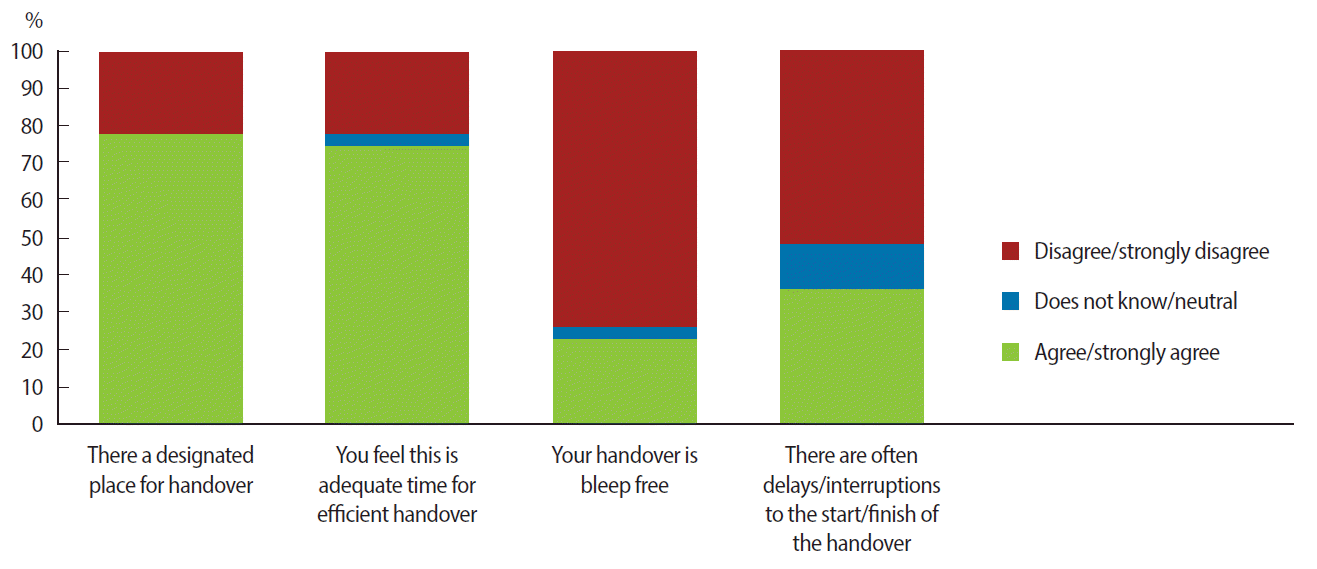
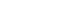
- All CSTs reported their units employed a shift-based on-call rota, as opposed to a 24-hour on-call system. CSTs reported that 5 units employed a ‘Surgeon of the Week’ system (i.e., on-call for 7 days or at least 4 days in a row). All shifts started between 07:00 and 08:30, and the majority (>80%) ended between 20:00 and 21:00. Only a few CSTs reported ending their shifts earlier than 20:00. A minimum of two handovers occurred per day, one in the morning (AM) and one in the evening (PM), and 22% of CSTs reported a third intra-day handover. Seventy seven percent of CSTs reported that their handover took place in a set location and lasted between 10 and 45 minutes. For AM and PM handovers only, 70% lasted 30 minutes or longer, and 74% of all CSTs deemed their handover duration to be adequate.
- For AM and PM handovers, 58% and 13% reported that the on-call consultant was in attendance at the handover, respectively. Moreover, 50% of CSTs reported that a designated health team member such as a consultant, a registrar, other CST, or senior nurse usually lead their handovers. Sixty-four percent confirmed that they had the opportunity to ask questions and clarify clinical issues with their colleagues and senior members of staff. Furthermore, 77% were satisfied with the quality of information received during the handover and 58% were satisfied with the degree of prioritisation of the information/clinical details conveyed during handover. All CSTs reported the use of computer-assisted printouts and patient lists during the handover. Twenty-two percent of trainees reported that their handovers were designated ‘bleep free’ (pager free), whereas 35% reported regular delays and interruptions during their handover sessions. AM handovers tended to be a multidisciplinary session attended by allied health staff (from the Nursing, Physiotherapy, Theatre, and Bed Management Departments) according to 50% of the CSTs, but only 28% reported that their PM handover was multidisciplinary (Fig. 1).
- Patient safety, maintenance, and educational value of handovers
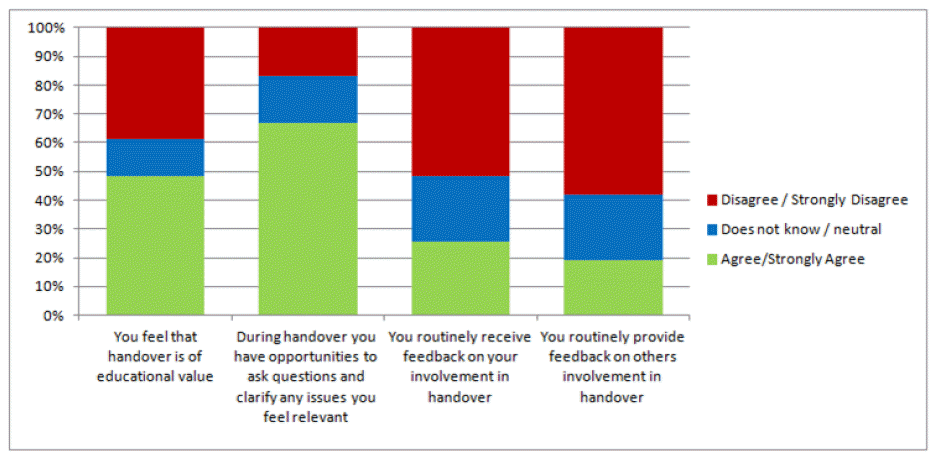
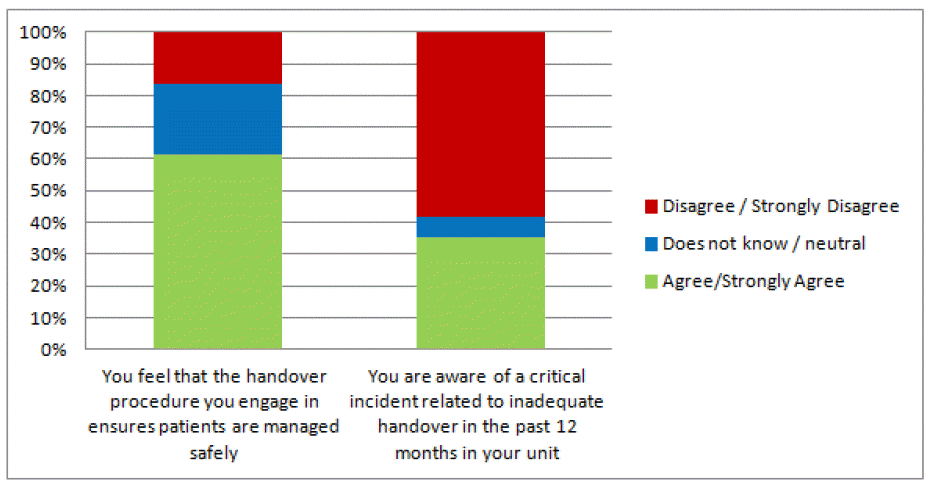
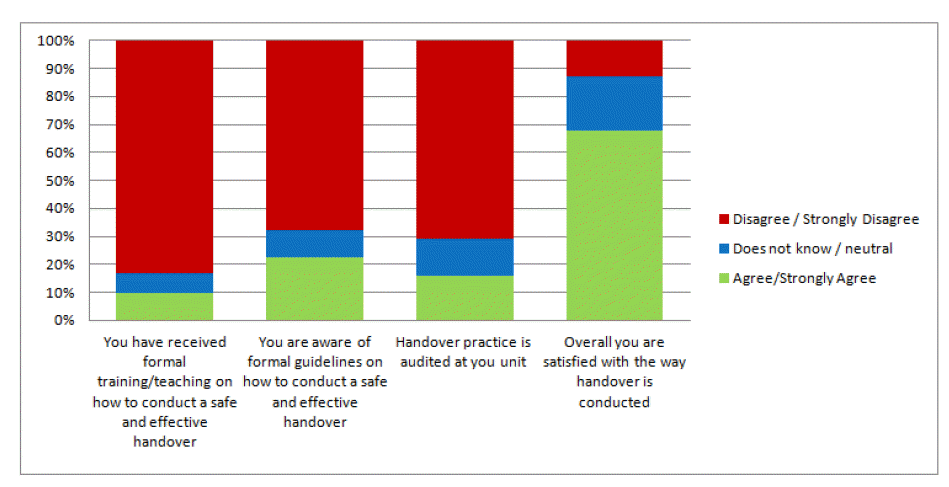
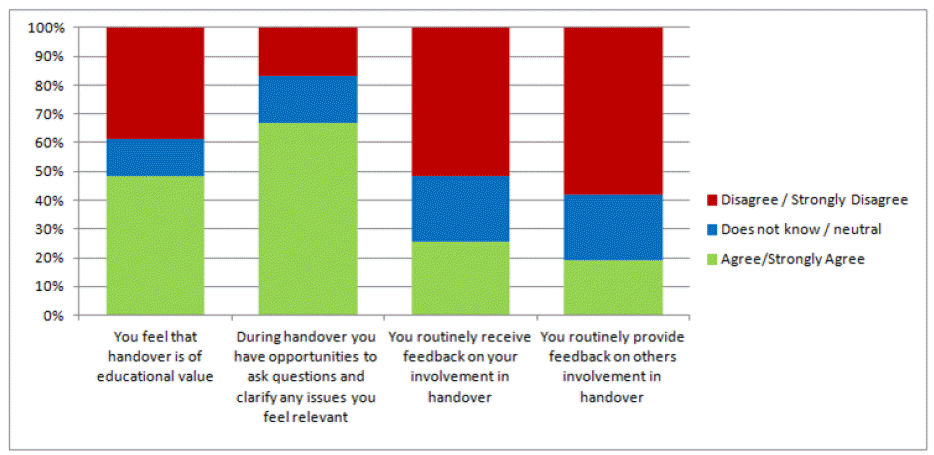
- Approximately a third of trainees (35%) were aware of a critical incident in the preceding twelve months related to inadequate handover practice. However, a majority (61%) of all CSTs felt their participation in the handover ensured that patients were managed safely and effectively, and 67% were satisfied with their practice of handovers (Fig. 2). Nearly half of all CSTs (48%) were aware of a formal handover policy for their designated unit, whilst only 20% reported to have received any formal training on how to conduct an effective handover. Furthermore, less than one quarter of CSTs (22%) were aware of the national guidelines on handover practice. In addition, the majority (84%) reported that handover practice was not audited in their unit (Fig. 3). Approximately half of CSTs (48%) felt that the handovers they engaged in were of educational value to their surgical training, and 38% of them strongly felt that handovers were of no educational value. Only 25% and 19% indicated they routinely provided or received feedback on each other's performance after performing a handover, respectively (Fig. 4).
RESULTS
- This is the first regional UK survey aimed at CSTs of all levels and from all surgical specialties that has targeted their practice and perception of handover in line with national recommendations. We targeted a specific category of trainees at the start of their surgical careers in the EWTD era. Only a few reports in the literature have documented the opinions of surgical trainees surrounding handover practice in the UK. These reports surveyed general surgical trainees (Northern Ireland)[7], burns trainees (UK)[8], and ENT trainees from several units (UK)[9]. A common theme amongst these reports was the shortcomings of handover practice within each specialty.
- In our regional study, only half of CSTs reported that an on-call consultant attended their AM handover regularly, and a lower proportion was found for the PM handovers, with a similar number reporting consultant-led handovers. The BMA guidelines state that daily involvement by senior clinicians is essential during handovers to ensure that appropriate clinical decisions are made, to demonstrate that handovers are taken seriously and are a vital part of patient safety, and to contribute to junior doctor education[1].
- Differences on the perceived value of handovers amongst senior consultants could be attributed to the lack of financial or hierarchical remuneration associated with handover attendance. For example, consultants whose contracts do not typically reward attendance and teaching at handover may not feel obliged to do so, particularly if a senior registrar is leading the handover process. Nevertheless, consultant attendance is also important in fostering cohesion within a unit and a team-based approach to clinical duties, therefore ensuring the sustainability of an effective handover process[10]. Consultants serve not only as leaders within their units and individual firms but also as mentors for their trainees. Moreover, they act as supervisors ensuring the competency of their trainees' actions, assuming overall responsibility for patient care, and coaching the clinical, professional, and educational development of their trainees.
- Despite CSTs reporting favourably on the safety of their handover practices, 35% also reported being aware of a ‘critical incident’ that stemmed from inadequate handover practice within the preceding 12 months. A recent study on clinical incidents amongst surgical patients at a UK hospital found that 6% of more than 300 reported clinical incidents over 3 years were likely due to inadequate handover practice[11]. Poor, incomplete, or no handovers for these patients were identified as the causes of inadequate care in three quarters of these cases. However, the reported severity and impact of these incidents were considered low in 99% of these cases, and reporting was anonymous and open to all members of staff. Thus, the frequency of reporting amongst surgical or medical trainees for these incidents of inadequate care is unknown. As a result, more critical or severe incidents may have been omitted, and this could have resulted in a reporting bias. In our study, further interpretation of incident reporting was difficult as a precise definition of 'a critical incident' was not provided in the questionnaire; therefore, our collected responses were amenable to experiential bias. In addition, some CSTs were working in the same units; therefore, the same incident could have been reported multiple times, thus reducing the accuracy of this measure.
- The BMA guidelines[1] state that handovers should be “interruption free” ; therefore, staff should refrain from interruptions due to telephone calls and bleeps/pages. However, most surveyed units in the UK do not suggest that handovers are interruption free[11-13]. In our survey, only 22% of CSTs reported a bleep-free environment at handover. Because patient safety is paramount, the on-call team must be contactable at all times in case of an emergency, which could explain why these results were apparent.
- Handover should be a multidisciplinary event, with involvement from all healthcare professionals including appropriate clinical and non-clinical staff[1]. However, only half of CSTs reported attending AM handovers that were multidisciplinary with allied health staff also in attendance, and an even smaller percentage reported a multidisciplinary PM session. CSTs were remarkably confident in the preservation of patient safety through their participation in handovers. Perhaps the team diligence amongst the CSTs and other staff to ensure patients were appropriately managed preserved patient safety and allowed patients to receive optimal care. CSTs could have been unaware of the standards that needed to be met in their practice and of the potential 'near misses' that could have been occurring in their units due to the lack of formal training administered at handover. Hence, these observations are noteworthy and deserve further study and audit, both regionally and nationally, to determine the nature of any reported adverse incidents and to determine units where practice could be improved.
- The majority of CSTs reported not receiving training on how to effectively perform a handover and were not aware of any formal guidelines for safe handover conduct. This finding reiterates recent observations from a large Scottish teaching hospital (composed of medical and surgical juniors, registrars, consultants, and nurse practitioners) that identified a vital need for the formal teaching of handover skills to junior doctors[12].
- A key observation in our study was the high level of dissatisfaction amongst CSTs regarding the perceived educational value of handovers. Trainees valued handover highly in terms of potential learning, but highlighted some educational deficiencies. This is likely to stem from a number of factors. A lack of formal training in handover processes, the absence of auditing of practice or outcomes, and discrepancies in regular and sustained consultant attendance (and hence leadership) may collectively serve to explain their perception of handover as being of low educational value. In the EWTD era, where opportunities for training have become concentrated, time-crucial and competency-based, all potential learning opportunities that are available for trainees should be exploited. The Royal College of Surgeons of England highlights that effective and high-quality handovers can be an “excellent training and review opportunity” that must be “maximised in a climate of shortened hours and streamlined training.” Despite acknowledgements of the potential educational benefits of formal handover sessions, there is a limited body of literature on the proposed methods of handover implementation in a trainee education programme in the UK[6[.
- Our results suggest the need for the introduction of several key initiatives at both the deanery and unit level. Through our experience we trialled and implemented these initiatives in one of our units (Department of Plastic&Reconstructive Surgery, John Radcliffe Hospital) (Fig. 5). Five CSTs rotated through this unit following these implementations and completed the questionnaire-based survey. All five CSTs reported improved satisfaction regarding training in handover, handover policy, in addition to a greater educational value from handover, and greater engagement within handover (data not shown). Although these are preliminary results, this is an interesting area to explore in further depth. The Oxford School of Surgery has since introduced formal handover training to CSTs at induction (at the start of their core training). At the time of commencing their surgical training, all new cohorts of CSTs will therefore be taught these formal guidelines, hopefully execute safe handovers, and utilise them as an important educational tool.
- Based on our experiences, we believe it should be made a priority for doctors to receive training and education on how to conduct a safe handover. This training may be most useful if conducted at the start of core training and then augmented through training with local surgical unit protocols. Trainees should be taught the reasons why safe and effective handovers are of importance, with a review of the national guidance. This training can be achieved through simple role-play scenarios, which appear to be a popular method to impart and practice requisite skills. Dedicated and consistent leadership by senior consultants during handovers is also needed to ensure trainees are supported and foster the handover experience as a potential daily learning opportunity. Efforts should also be made to encourage a multidisciplinary approach to handover, integrating with allied specialties, and encouraging attendance by all those who are most closely involved in patient care. Logistically this may be difficult to arrange with the staggered arrangements of surgical and nursing handovers, but may perhaps only require attendance by only one chosen nurse who can voice important patient issues at handover, relaying pertinent information back to nursing colleagues. Lastly, effective handovers lead to optimal patient continuity of care; therefore, further investigations to examine patient outcomes in light of handover practice, identifying potential deficiencies, and guiding best practice are needed.
- This survey was limited by the small number of participants, albeit they represented 80% of the CSTs in the region, were from multiple hospitals, and represented six surgical specialties. We cannot rule out the potential for a reporting bias (where CSTs reported what they felt took place at handover as opposed to what actually took place), and selection bias (where we looked at CSTs only and not registrars or consultants. Nevertheless, this UK study targeting CSTs in the EWTD era highlighted that current handover practice is compliant with national guidelines; however, its educational value should be targeted, improved, and used as a tool to maximise educational opportunities among trainees.
DISCUSSION
SUPPLEMENTARY MATERIAL
-
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported
Article information

- 1. National Patient Safety Agency. Safe handover: safe patients. Guidance on clinical handover for clinicians and managers [Internet]. London: British Medical Association; [cited 2014 Mar 24]. Available from: http://bma.org.uk/-/media/files/pdfs/practical%20advice%20at%20work/contracts/safe%20handover%20safe%20patients.pdf
- 2. Waurick R, Weber T, Broking K, Van Aken H. 20:576-579. http://dx.doi.org/10.1097%2FACO.0b013e3282f0ef61
- 3. The Royal College of Anaesthetists. A compendium of solutions for implementing the working time directive for doctors in training from August 2009 [Internet]. London: The Royal College of Surgeons of England; 2009 [cited 2013 Sep 5]. Available from: http://www.rcoa.ac.uk/document-store/compendium-of-solutions-implementing-the-working-time-directive-doctors-training
- 4. The Royal College of Surgeons of England. Good surgical practice 2008 [Internet]. London: The Royal College of Surgeons of England; 2007 [cited 2013 Sep 5]. Available from: http://www.rcseng.ac.uk/publications/docs/good-surgical-practice-1
- 5. The Royal College of Surgeons of England. Safe handover: guidance from the working time directive working party [Internet]. London: The Royal College of Surgeons of England; 2007 [cited 2013 Sep 5]. Available from: http://www.rcseng.ac.uk/surgeons/surgical-standards/docs/Safe%20handovers.pdf/view
- 6. Klaber RE, Macdougall CF. Maximising learning opportunities in handover. Arch Dis Child Educ Pract Ed 2009;94:118-122. http://dx.doi.org/10.1136/adc.2008.142471 ArticlePubMed
- 7. Kennedy R, Kelly S, Grant S, Cranley B. Northern Ireland general surgery handover study: surgical trainees' assessment of current practice. Surgeon 2009;7:10-13. http://dx.doi.org/10.1016/S1479-666X(09)80060-7 ArticlePubMed
- 8. Al-Benna S, Al-Ajam Y, Alzoubaidi D. Burns surgery handover study: trainees' assessment of current practice in the British Isles. Burns 2009;35:509-512. http://dx.doi.org/10.1016/j.burns.2008.11.008 ArticlePubMed
- 9. Karnwal A, Ho EC, Pakalapati SS, Tyagi M. A survey of handover practices among ENT units in England. Clin Otolaryngol 2008;33:380-381. http://dx.doi.org/10.1111/j.1749-4486.2008.01711.x Article
- 10. Hannan TJ, Bart S, Sharp C, Fassett MJ, Fassett RG. The sustainability of Medical Morning Handover Reporting: adherence in a regional hospital. Aust Health Rev 2010;34:325-327. http://dx.doi.org/10.1071/AH09820 ArticlePubMed
- 11. Pezzolesi C, Schifano F, Pickles J, Randell W, Hussain Z, Muir H, Dhillon S. Clinical handover incident reporting in one UK general hospital. Int J Qual Health Care 2010;22:396-401. http://dx.doi.org/10.1093/intqhc/mzq048 ArticlePubMed
- 12. Cleland JA, Ross S, Miller SC, Patey R. "There is a chain of Chinese whispers...": empirical data support the call to formally teach handover to prequalification doctors. Qual Saf Health Care 2009;18:267-271. http://dx.doi.org/10.1136/qshc.2008.029983 ArticlePubMed
- 13. Jeffcott SA, Evans SM, Cameron PA, Chin GS, Ibrahim JE. Improving measurement in clinical handover. Qual Saf Health Care 2009;18:272-277. http://dx.doi.org/10.1136/qshc.2007.024570 ArticlePubMed
References
Appendix
Appendix
Figure & Data
References
Citations


 KHPLEI
KHPLEI

 PubReader
PubReader ePub Link
ePub Link Cite
Cite