Articles
- Page Path
- HOME > J Educ Eval Health Prof > Volume 9; 2012 > Article
-
Research Article
Strengthening the admissions process in health care professional education: focus on a premier Pacific Island medical college -
Christian Chinyere Ezeala1*
 , Mercy Okwudili Ezeala2, Niraj Swami3
, Mercy Okwudili Ezeala2, Niraj Swami3 -
Journal of Educational Evaluation for Health Professions 2012;9(11):1-6.
DOI: https://doi.org/10.3352/jeehp.2012.9.11
Published online: November 30, 2012
1Department of Health Science, College of Medicine, Nursing and Health Sciences
2Department of Communication and Language and Literature, College of Humanities and Education
3Health Professions Education Unit, College of Medicine, Nursing and Health Sciences, Fiji National University, Fiji
- *Corresponding email: christian.ezeala@fnu.ac.fj
© 2012, National Health Personnel Licensing Examination Board of the Republic of Korea
This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 30,689 Views
- 156 Download
- 3 Crossref
Abstract
- Relying solely on measures of intellectual aptitude and academic performance in university admissions can be disadvantageous to underprivileged students. The Fiji School of Medicine primarily uses such measures to evaluate and select student applicants, and the introduction of supplementary assessments could provide better access for students from disadvantaged backgrounds. This study examined the need for supplementary assessments in the admission process, types of additional assessments needed, and stakeholders’ views on a multi-entry multi-exit strategy currently in use at the Fiji School of Medicine. A survey of the key stakeholders was conducted in February and March 2012 using closed and open ended questionnaire. One hundred and twenty-two validated questionnaires were self-administered by key stakeholders from the College of Medicine, Nursing and Health Sciences (CMNHS) and Fiji Ministries of Education and Health, with a response rate of 61%. Returned questionnaires were analysed quantitatively and qualitatively. Sixty-five percent of respondents supported the introduction of supplementary assessments, 49% favoured admissions test, and 16% preferred assessing non-academic factors. Many respondents supported the School’s multi-entry multi-exit strategy as a ‘good policy’ that provided ‘flexibility’ and opportunity for students, but should be better regulated. These findings demonstrate the need for supplementary assessments in the selection process and for continued support for the use of multi-entry multi-exit strategy at the school.
- A major challenge facing health professional educational institutions around the world today is selecting and admitting students that will successfully complete their course of study in a timely manner. This challenge also extends to the need to produce capable practitioners that will make positive contributions to the development of health care in their communities. An underlying concern in student selection is choosing which candidates will have a high probability of success in their programme while also giving access to candidates from underprivileged backgrounds. The need to select the best students must be balanced with consideration for equity issues without unduly undermining the quality of admissions. This is particularly crucial for institutions that serve diverse populations such as the Fiji School of Medicine. The World Federation for Medical Education (WFME) weighed in on these issues, among other things, in its global standard for quality improvement in basic medical education: “The admission policy should be reviewed periodically, based on relevant societal and professional data, to comply with the social responsibilities of the institution and the health needs of the community and society…The needs of community and society may include the consideration of balanced intake according to gender, ethnicity and other social factors, including the potential need for a special admission policy for underprivileged students” [1].
- Since its inception in 1885, the Fiji School of Medicine has remained a prominent regional health professional educational institution in the South Pacific, training much of the health care labour pool throughout the small island countries and surrounding territories [2,3]. Now a part of the College of Medicine, Nursing and Health Sciences (CMNHS) of the Fiji National University, it selects its students through the use of measures of cognitive ability, such as their Form 7 score on the Fijian high school examination, on their cumulative grade point average (CGPA) in the remedial ‘Foundation Studies’ organized by some universities, or based on their academic performance in an undergraduate programme.
- Both measures focus on the cognitive abilities of the candidates. Although a recent study by Ezeala et al. [4] demonstrated that high school scores were highly predictive of academic success in the first year of the Bachelor of Medicine and Bachelor of Surgery (MBBS) undergraduate degree programmes at the Fiji School of Medicine, several research reports in the literature show that intellectual aptitude is not the sole determining factor of success in medical education and in professional practice; inevitably, non-cognitive psychosocial factors play key roles [5–7]. No studies have demonstrated the validity of the entry scores in predicting a student’s success in any of the school’s programmes or in determining their professional performance as qualified health care practitioners upon graduation. Some of the non-cognitive factors listed in the literature that are known to influence academic and professional performance include a positive self-concept, realistic self-appraisal, demonstrated leadership potential, availability of a strong support person, ability to handle ethnic and racial differences, making and working towards long-term goals, and a commitment to community service [8–11]. There should also be a way to evaluate these characteristics when selecting students who will complete their studies and become health care professionals.
- One particular feature of student admissions for some of the Fiji School of Medicine’s programmes is the multi-entry multi-exit strategy, which allows students to exit an academic programme mid-way with a certificate or diploma, and ultimately returning to complete their degree requirements after some years. As laudable as this policy appears, it is in need of a review and evaluation. This study was designed to analyze whether there is need to introduce supplementary assessment procedures for admissions into the Fiji School of Medicine, as well as to determine the types of assessments that might be required and to explore the views of the current stakeholders in the school’s multi-entry multi-exit strategy presently adopted by the School in some of her programmes.
INTRODUCTION
- A survey was conducted in February and March 2012 to determine the views of stakeholders on the admissions processes of the Fiji School of Medicine of the Fiji National University. The College Health Research and Ethics Committee (CHREC) of the CMNHS approved the proposal and the Department of Health Sciences Research Committee earlier gave clearance to conduct the study. A questionnaire was then developed and validated by issuing it to 20 academic and 10 administrative staff in the CMNHS to determine the construct validity of each question. The questionnaire contained six multiple choice questions and one open-ended question (Appendix 1). Since the sole purpose of the pilot test was to validate the instrument, the results of the pilot test were not included in the main study.
- Once the questionnaire was developed, the main study polled key policy stakeholders drawn from the CMNHS, the Ministry of Education, and the Ministry of Health. It was assumed that these subjects had better awareness of the medical school’s admission processes and policies, and were thus in a better position to influence the decision making processes. As the intent of the study was to include as many of the key stake-holders as possible, 122 questionnaires were issued to all the accessible key stakeholders at the time of the study. Participants were informed of the nature and purposes of the study and they voluntarily gave consent to participate in the study. Participants were instructed to complete their questionnaires at their convenience and to respond to the questions and comments as truthfully as possible. The questionnaires were followed up by personal visits and/or phone calls to the subjects by the researchers.
- The returned questionnaires were analysed quantitatively to produce simple proportions, and the results have been expressed as percentages. Inductive coding was used to analyse the qualitative survey responses. Two independent qualitative analysts used open inductive coding to generate descriptive codes that were then harmonized and sorted into coding frames. The resultant coding frames were then re-applied to each text to deductively recode the original data along specific ‘themes.’
MATERIALS AND METHODS
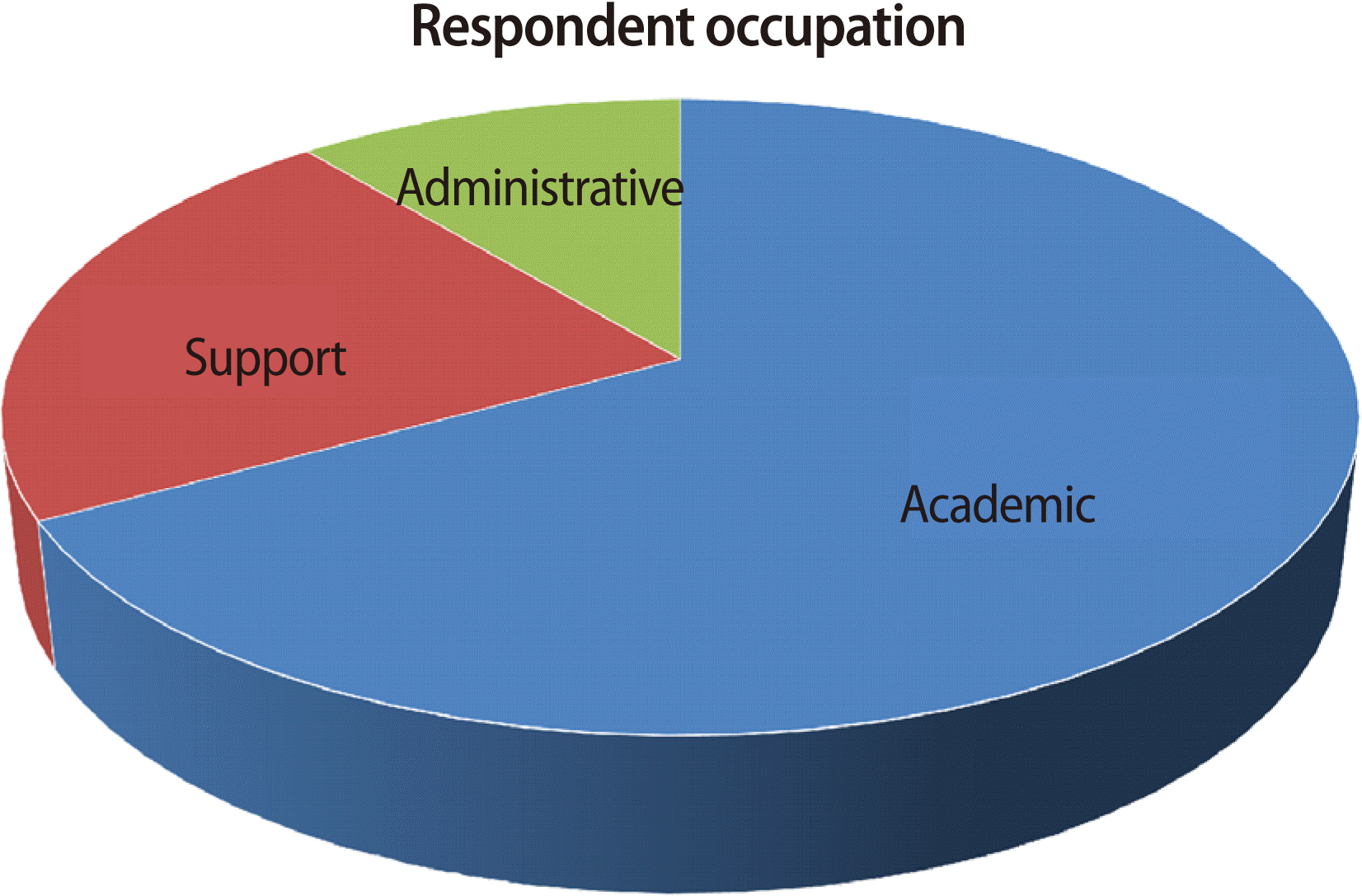
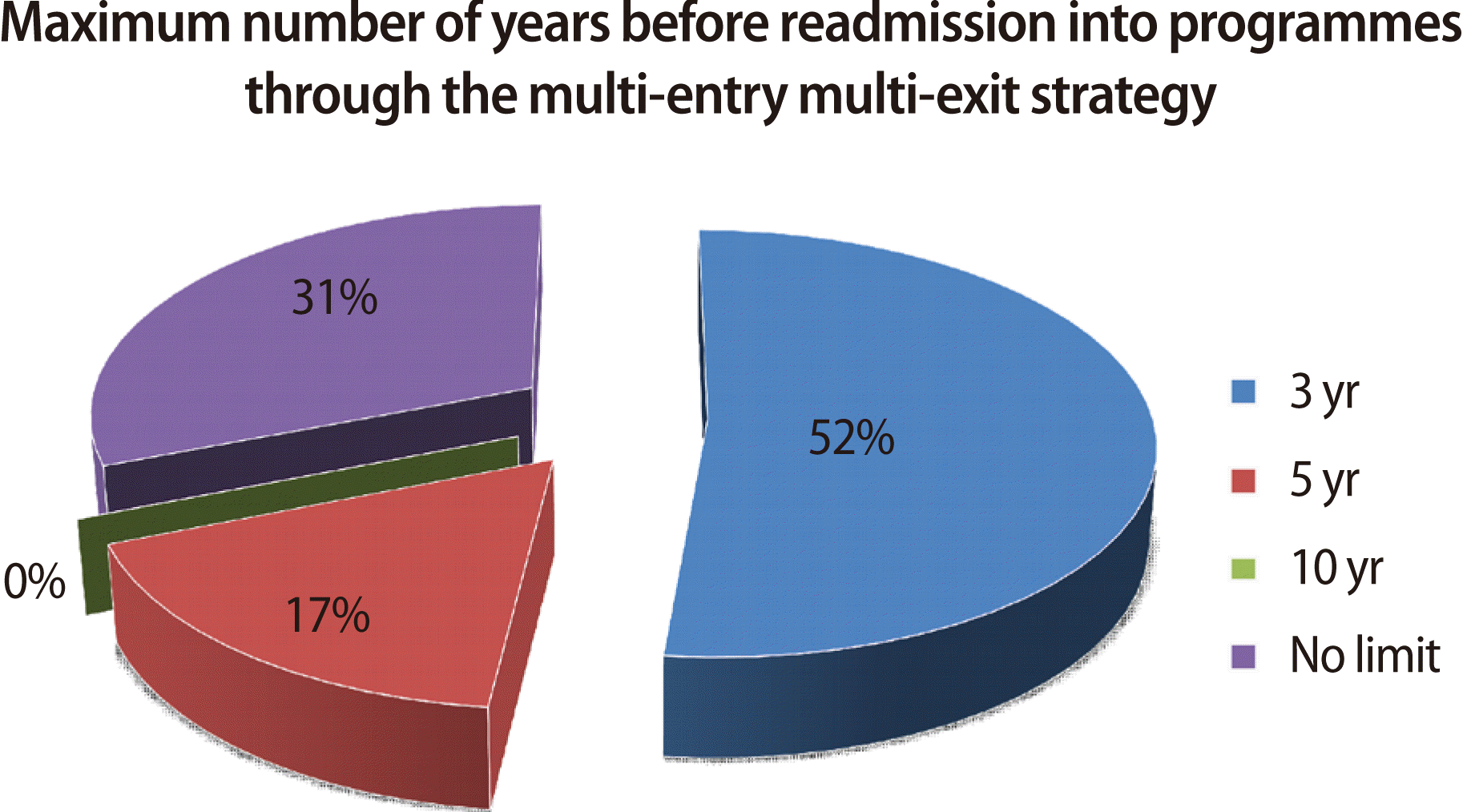
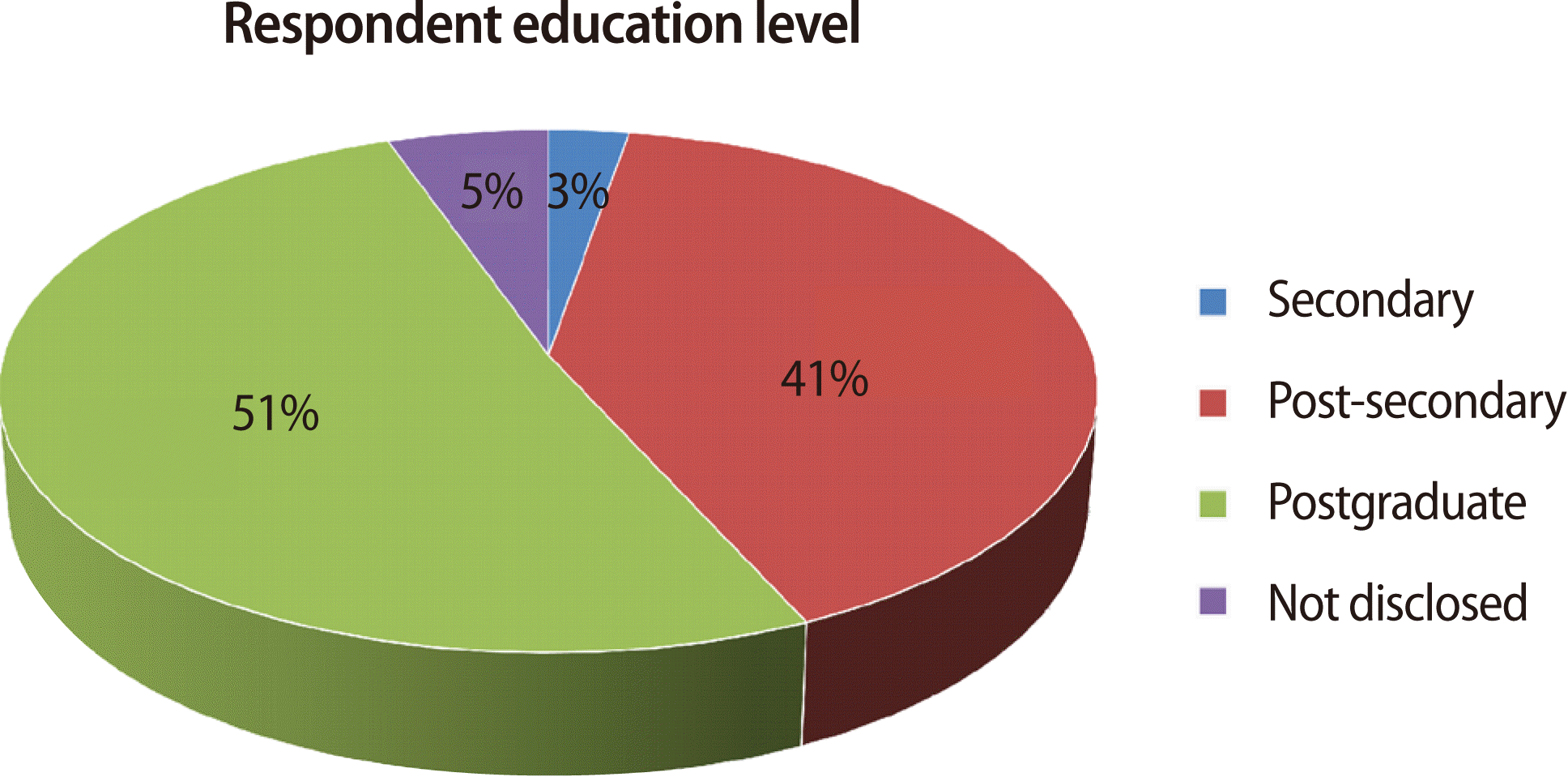
- Of the 122 questionnaires issued to the respondents only 74 were completed and returned, giving a response rate of 61%. Fig. 1 shows that a majority of the respondents held academic positions, with participants in administrative or supporting staff roles comprising the remainder. Over 5% of the respondents held both administrative and academic positions. Of the 74 respondents, 78.4% were staff of the CMNHS, 13.5% were from the Ministry of Education, and 8.1% were from the Ministry of Health. Fig. 2 shows the education levels of the respondents. The data in Table 1 show that 65% of the respondents supported the introduction of supplementary assessments for admissions into the School. Forty-nine percent favoured the use of a formal college admissions test, 16% preferred a focus on non-cognitive factors, while the others recommended a formal interview of the candidates. Many of the respondents supported the multi-entry multi-exit strategy as a “good policy” that offered flexibility and opportunity to students to plan their studies in a manner that might better suit their financial and social needs. A sample of respondents’ positive comments follows:
- “Excellent (idea), offers opportunities to create a career path, to plan studies, and …”
(Department of Oral Health academic and administrative staff)
- “I think it is a good policy…it provides for graduating students according to the level of their abilities. It also ensures that intermediate to mid-level manpower can be produced in the College to service the health care industry in the Pacific Island Countries ”
(CMNHS academic)
- Several respondents, however, cautioned that this program could be vulnerable to abuse and that proper regulation should be in place to monitor its effective implementation. Respondents also emphasized that students terminated on grounds of poor academic performance should not be readmitted into the same programme at a later date:
- Some respondents expressed the belief that a medical student terminated during their clinical years of study (years 4 to 6) should be awarded a Bachelor of Medical Science degree if he or she successfully completed the preclinical curriculum, instead of leaving students in such an instance without any academic reward for their efforts.
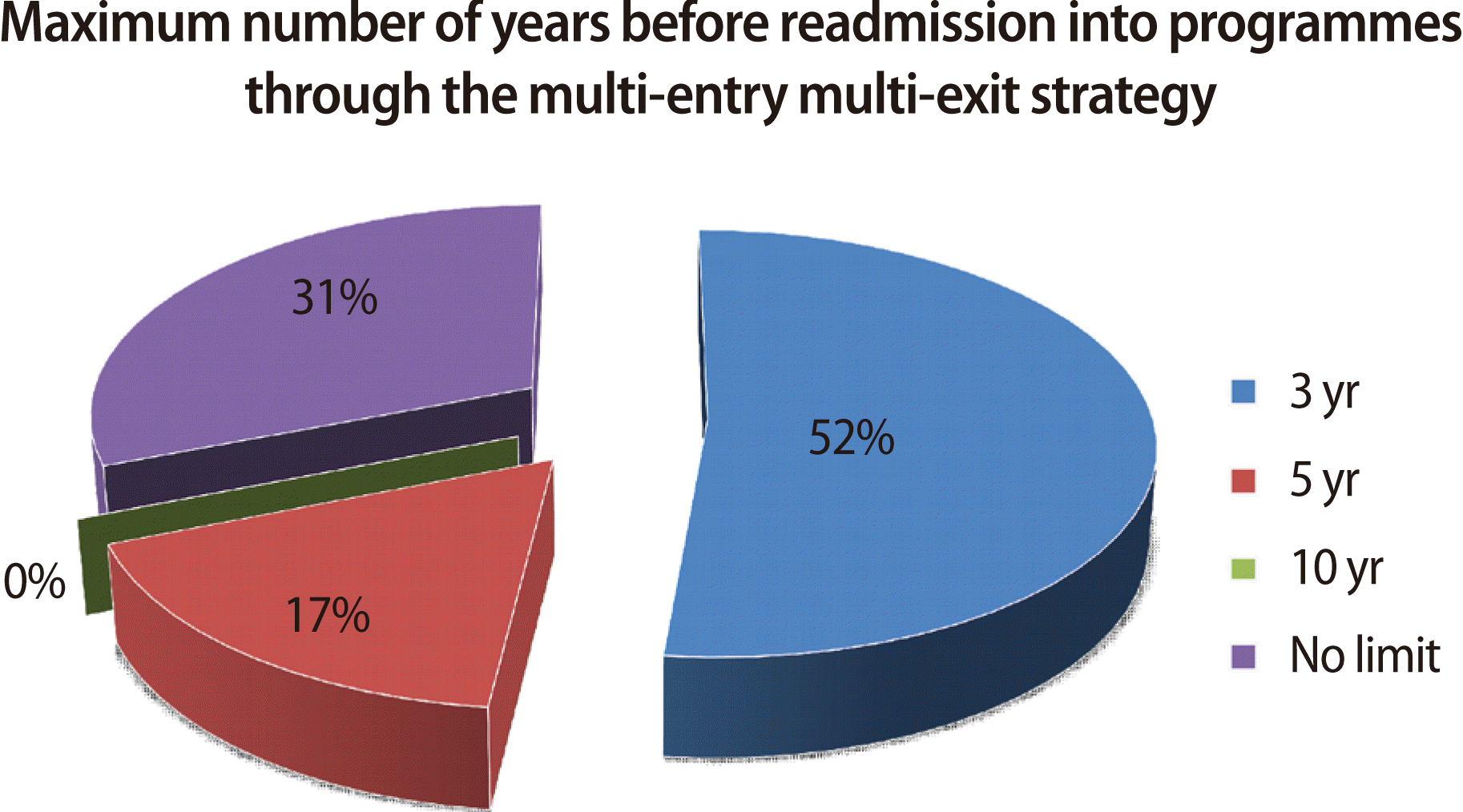
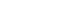
- Fifty-two percent of the respondents were of the opinion that students should not be readmitted into a programme if more than three years have elapsed since their last formal education in that programme. Seventeen % favoured a maximum interval of five years between exit and re-entry. Thirty-one percent preferred no set time limit for readmission. Fig. 3 shows the full scope of responses.
RESULTS
- The Fiji School of Medicine is a regional health professional educational institution with a mission to provide medical training and research facilities to the Pacific Islands region. This geographic region is characterized by ethnic, religious, generational, cultural, and socio-economic diversity. Given this reality, limiting selection criteria to purely quantitative academic performance data is effectively a policy of restriction because it disproportionately disadvantages candidates from under-privileged backgrounds, who may possess desirable characteristics required for a successful career in health care, but who face many barriers to accessing higher education [12]. Results from this study showed that nearly two-thirds of respondents supported the introduction of supplementary assessments for student selection, and nearly one-half favoured the use of a university/college admissions test.
- The question remains then as to the nature of college admissions tests and how they should be organized at the Fiji School of Medicine. Given that the respondents were aware of the results of the study by Ezeala mentioned above [4], which showed that the current criteria used in the college strongly predicted academic performance in the first year, it could be argued that these respondents were not just calling for another measure of intellectual aptitude, but rather they were calling for an assessment that would address other characteristics of the candidates that affect academic and professional performance. In the process of doing this, the school might improve access to some underprivileged applicants whose background may not have been conducive to a high score on the high school tests, but would nonetheless make excellent students. This supposition is given further weight when we take into account the significant respondent support for the use of non-academic variables and personal interviews during the admissions process. True, the adoption of this proposal may require elaborate preparation, staff training, and may pose financial and administrative challenges. However, it could also potentially lead to a greater sense of legitimacy around the school’s admissions procedures.
- This view has been emphasized by Sedlacek et al. [10,11] and has for a long time been adopted by universities and scholarship granting organizations in North America [13]. The various means of assessing non-academic variables could be organized into a holistic admissions process. There are a number of possible alternatives to simply measuring academic performance, including the use of a structured questionnaire such as the standard Non-Cognitive Questionnaire (NCQ), students submitting a learning or life experience portfolio, and face-to-face personal interviews [10]. A validated Multiple Mini-Interview (MMI) scheme, such as the one originally developed by McMaster University [14], which is similar to the Objective Structured Clinical Examination (OSCE), would conform to the dictums of problem-based learning currently adopted by the Fiji School of Medicine in some of its programmes. Medical Schools in the United States, Canada, and Australia are already successfully using such tests for the selection of their students [15–17].
- It should be understood that this is not an advocacy for the lowering of admission standards, but rather widening of the scope of assessments to honour a variety of important characteristics in students and to improve access for candidates from disadvantaged backgrounds. The high level of support for the School’s multi-entry multi-exit strategy is worth noting again. This strategy is believed to provide improved access to indigent students or students with other life or financial constraints. Nonetheless, it requires evaluation and oversight to determine the retention rate of students readmitted on this basis and their eventual performance as health professionals following graduation. This could be an interesting area of future study. For example, the findings of this study could be a jumping off point for a policy review over whether to limit to five years the maximum interval between exit and re-entry for students.
- The limitation of this study is that only the key stakeholders were studied, and this could introduce many different biases that are not easy to quantify. We felt that the sample was valid in light of the potential bias because the surveyed key stake-holders had a better understanding of the intricacies of health care professional education in Fiji and the Pacific Islands, and were thus in a better position to provide nuanced and informed responses to our questions.
DISCUSSION
Acknowledgments
-
This article is available from: http://jeehp.org/
-
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
Article information
| Question | Response (%) | |
|---|---|---|
| Additional assessment is required | Strongly agree | 29.7 |
| Agree | 35.1 | |
| No opinion | 5.4 | |
| Disagree | 18.9 | |
| Strongly disagree | 10.8 | |
| Type of additional assessment needed | College admissions test | 48.6 |
| Non-Academic factors | 16.2 | |
| Age of applicant | 8.1 | |
| Time elapsed since last formal education | 8.1 | |
| Other* | 3.5 | |
- 1. World Federation for Medical Education. Basic medical education: WFME global standards for quality improvement Copenhagen: World Federation for Medical Education; 2003 [cited 2012 Jun 28]. Available from: http://www.wfme.org/standards/bme. PubMed
- 2. Rouse I. The ‘regional’ medical school in Fiji: 125 years young – what an amazing journey. Pac Health Dialog 2010;16:5-6.
- 3. Ezeala CC. 125 years of health professions education at the Fiji School of Medicine. 2010 [cited 2012 Jul 19]. Available from: http://www.faimer.org/education/fellows/observations.html#cezeala.
- 4. Ezeala CC. Admission scores as a predictor of academic success in the Fiji School of Medicine. J High Educ Police Manag 2012;34:61-6. Article
- 5. Tracey TJ, Sedlacek WE. Factor structure of the noncognitive questionnaire- revised across samples of black and white college students. Educ Psychol Meas 1989;49:637-48. Article
- 6. Smits PB, Verbeek JH, Nauta MC, Ten Cate TJ, Metz JC, van Dijk FJ. Factors predictive of successful learning in postgraduate medical education. Med Educ 2004;38:758-66. ArticlePubMed
- 7. Lynch CD, McConnell RJ, Hannigan A. Dental school admissions in Ireland: can current selection criteria predict success? Eur J Dent Educ 2006;10:73-9. ArticlePubMed
- 8. Fuertes JN, Sedlacek WE. Using noncognitive variables to predict the grades and retention of Hispanic students. Coll Stud Aff J 1995;14:30-6.
- 9. Bandalos D, Sedlacek W. Predicting success of pharmacy students using traditional and non-traditional measures by race. Am J Pharm Educ 1989;53:145-8.
- 10. Sedlacek WE. Beyond the big test: noncognitive assessment in higher education. San Francisco: Jossey-Bass; 2004.
- 11. Sedlacek WE. Why we should use noncognitive variables with graduate and professional students. The Advisor 2004;24:32-9.
- 12. Wilks J, Wilson K. Going on to uni? Access and participation in university for students from backgrounds of disadvantage. J High Educ Policy Manag 2012;34:79-90. Article
- 13. Sedlacek WE, Sheu HB. The academic progress of undergraduate and graduate Gates Millennium Scholars and non-scholars by race and gender. Read Equal Educ 2008;23:143-177.
- 14. Eva KW, Rosenfeld J, Reiter HI, Norman GR. An admissions OSCE: the multiple mini-interview. Med Educ 2004;38:314-26. ArticlePubMed
- 15. Sedlacek WE. Employing noncognitive variables in selecting and developing students in higher education [Internet]. 2011 [cited 2012 Jun 28]. Available from: http://www.nacacnet.org/events/critical/Documents/EmployingNoncognitiveVariables.pdf.
- 16. Sedlacek WE. Using noncognitive variables in assessing readiness for higher education. In: Bowman PJ, St John EP, Stillman PK, editors. Diversity, merit, and higher education: toward a comprehensive agenda for the 21st century. New York: AMS Press; 2011. p. 187-206.
- 17. Harris S, Owen C. Discerning quality: using the multiple mini-interview in student selection for the Australian National University Medical School. Med Educ 2007;41:234-41. ArticlePubMed
References
Appendix
Appendix 1
Q1. Please state where you work __________________________________
Q2. Which of the following best describes your work?
Q3. Which of the following levels of education describes your highest qualification?
Q4. Based on the information provided in the information sheet, do you agree that supplementary assessments should be introduced for selection of students into the programmes of the Fiji School of Medicine?
Q5. If you agree to the use of additional criteria for student selection, which of the following would you recommend?
Q6. State your views on the multi-entry multi-exit policy of the college
Q7. With the multi-entry multi-exit strategy, what do you think should be the maximum duration for re-entry into a programme since the last exit?
Figure & Data
References
Citations

- Identification of the components for investigation of the psychological strength of nursing applicants: A qualitative study
Farzaneh Bagheriyeh, Akram Ghahramanian, Leila Valizadeh, Vahid Zamanzadeh, Geoffrey Dickens
Nursing Open.2022; 9(6): 2618. CrossRef - A scoping review of admission criteria and selection methods in nursing education
Vahid Zamanzadeh, Akram Ghahramanian, Leila Valizadeh, Farzaneh Bagheriyeh, Marita Lynagh
BMC Nursing.2020;[Epub] CrossRef - The New Era of : What Should Be Prepared to Be a Top Journal in the Category of Gastroenterology and Hepatology
Sun Huh
Journal of Neurogastroenterology and Motility.2013; 19(4): 419. CrossRef

 KHPLEI
KHPLEI


 PubReader
PubReader ePub Link
ePub Link Cite
Cite